Healthcare costs have become such a crushing burden that millions of people worldwide are making impossible choices between their health and their financial survival. While medical bankruptcy has become synonymous with the American healthcare nightmare, the reality extends beyond U.S. borders, creating ripple effects that touch families across continents. The fear of devastating medical bills now shapes healthcare decisions in ways that would have been unthinkable just decades ago.
United States

The United States leads the world in medical bankruptcies, with 530,000 American families filing for bankruptcy due to medical bills annually, making medical expenses directly cause 66.5% of bankruptcies. One in four adults with health coverage struggle with high out-of-pocket costs, and many Americans don’t get needed prescriptions filled and skip ongoing care, causing their health problems become worse and more costly to treat. Stories like Astrid Storey’s are becoming increasingly common, as her monthly premiums under the Affordable Care Act will jump by nearly $500 in 2026, while Nathan Boye faces premiums soaring from $28 to more than $700. The financial terror is so severe that people are genuinely contemplating abandoning their American dreams or giving up on healthcare entirely.
Canada

While Canada has universal healthcare, 19% of clients still cite illness, injury and health-related problems as a cause of their financial difficulties, with 15% of senior Canadians of at least 55 years naming medical reasons as the primary cause of insolvency. Despite universal health care in Canada, people are filing bankruptcy for medical reasons because financial trouble starts with time off work recovering from their health problems, during which they use credit to survive and pay day-to-day bills, leaving them with more debt than they can handle once they return to work. The hidden costs of being sick, like lost wages and extended recovery periods, create financial devastation even when the actual medical care is free.
United Kingdom

Medical bills bankruptcy statistics from 2005 show that 8.2% of those that went bankrupt in the UK listed illness or accident as the reason, according to data from the former Insolvency Service. When you have an illness that requires a major operation in Britain, you are likely to end up on a long waiting list, and if the illness renders you unable to work, then the longer you are on the waiting list the more your finances will be strained. Patients in The UK often face far longer wait times for care, particularly “elective” care, than those in the US. The cruel irony of the NHS system reveals itself when free healthcare becomes financially devastating through delays that destroy livelihoods while patients wait for treatment.
Australia
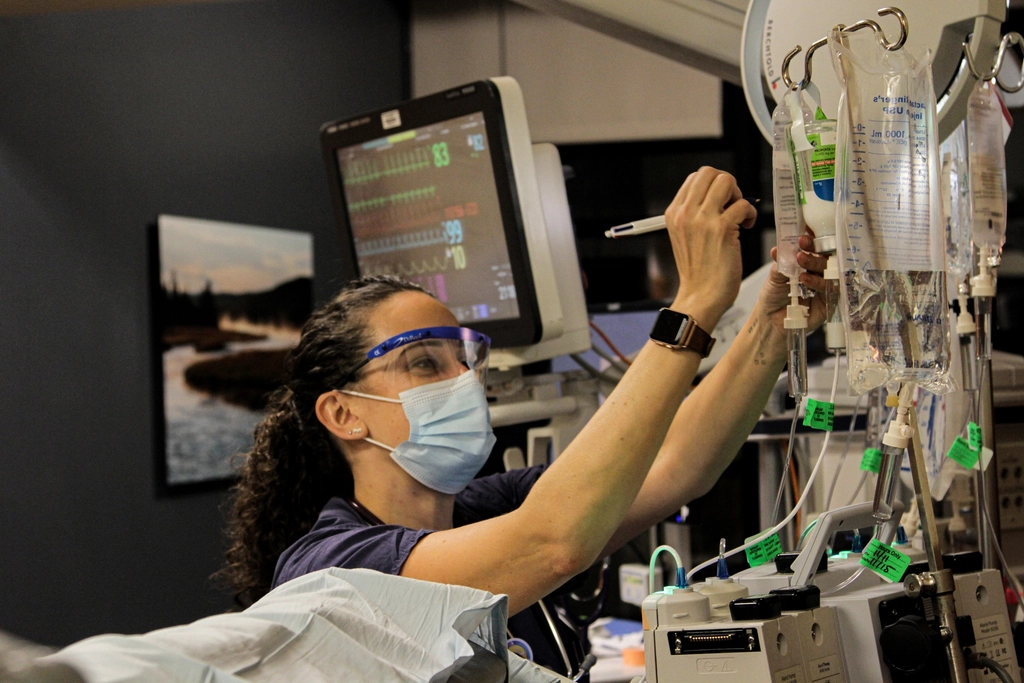
In the fiscal year 2016-2017, Australia saw a total of 25,225 personal insolvencies, among which about 1,830 resulted from health conditions, meaning only 7.25% of all personal insolvencies are related to medical issues. According to 2016/17 stats from the Australian Government, 1,830 of the 25,225 personal insolvencies were caused by ill health, and since Australia has universal healthcare like Canada and the UK, medical related bankruptcies result from loss of income around an illness rather than from the cost of care itself. Even in a country with robust universal coverage, the economic impact of illness continues to push thousands into financial ruin through lost productivity and extended recovery periods.
Germany
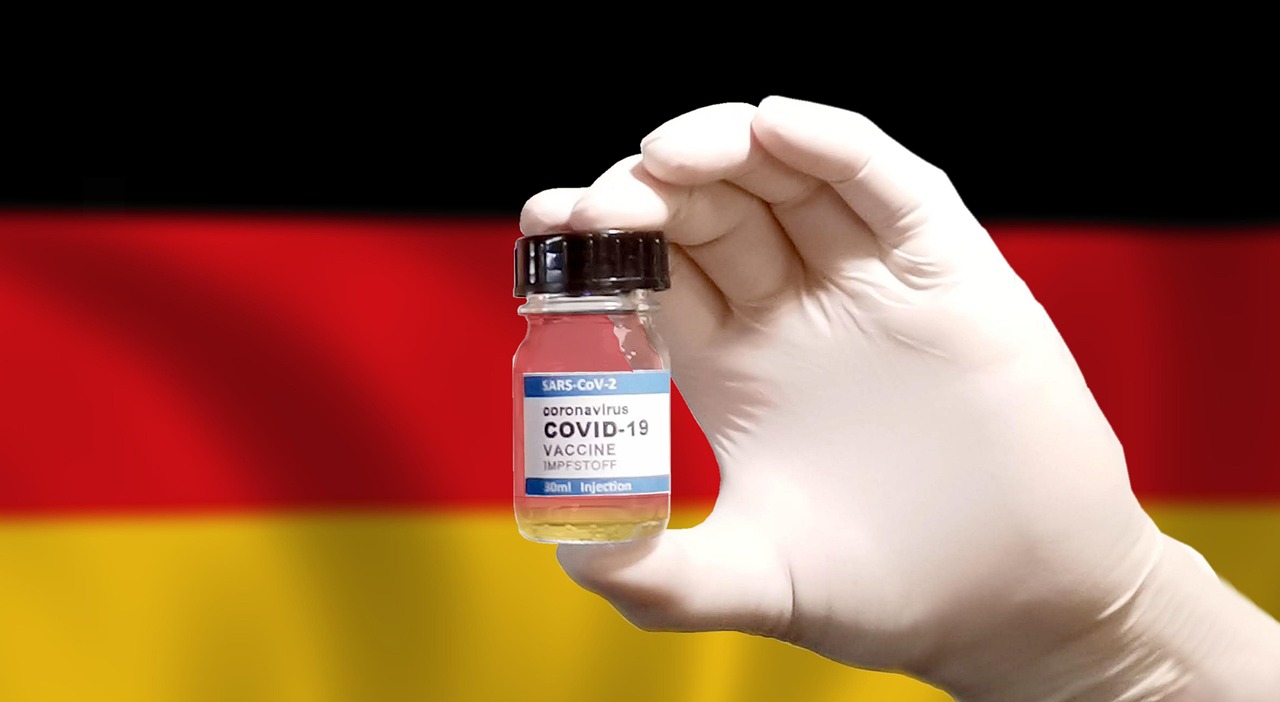
Germany operates a universal multi-payer healthcare system, primarily funded through statutory health insurance, ensuring comprehensive coverage for all citizens. Healthcare spending in Germany was 11.2% of GDP in 2014, with 74% of that being from public programs and 13.2% from out-of-pocket spending, mostly on nursing homes, pharmaceuticals, and medical aids, with costs contained primarily through emphasizing quality and efficiency. Providers are generally much better paid in the US, which is a major driver behind our higher costs, but it also helps prevent the strikes and demonstrations for high pay sometimes seen in Germany and elsewhere. Even Germany’s celebrated healthcare system struggles with provider compensation issues that can disrupt care delivery when workers demand better wages.
China

China is notably mentioned as an exception among developed economies, as other developed economies have single-payer health care systems where medical costs are financed by taxes, not by premium-financed insurance. After the Chinese economic reform in 1978, the state reduced spending on hospitals and allowed them to charge patients for profit, and from the high point of privatization of healthcare in the 1990s, China has been reforming with universal health care as a goal in the twenty-first century. China’s “Law on Promotion of Basic Medical and Health Care”, effective June 2020, asserts that Chinese citizens have a positive right to healthcare, regardless of cost. China’s healthcare transformation represents one of the most dramatic shifts from privatized chaos back toward universal coverage, driven by the recognition that market-based healthcare devastated millions of families.
Switzerland

Universal coverage was introduced in Switzerland through the Federal Health Insurance Law in 1996 with three goals: universal coverage with low-income subsidies, comprehensive and high quality coverage, and containment of growing health care costs, administered by 26 individual cantons with financing coming from general tax revenues and Mandatory Health Insurance premiums. Switzerland entirely eliminates government entitlement programs like Medicare and Medicaid with everyone on private insurance from birth to death, with plans tightly regulated and decoupled from employment, though out-of-pocket expenses are relatively high to combat moral hazard. The Swiss model proves that even with universal coverage mandates, high out-of-pocket costs can still create barriers that make people think twice before seeking necessary medical care.
France
An article by Stanford Medicine compares the US medical bankruptcy statistics with those of France, highlighting that in 2007, 62% of all US insolvencies resulted from medical costs, while by contrast, in France, there were no medical-related bankruptcies in 2008. The main reason is the single-payer system that ensures everyone gets free healthcare, though Stanford Medicine highlights that taxation in France is much heavier than in the USA. France’s healthcare system is insurance-based, offering universal coverage with a mix of public and private providers, funded by mandatory health insurance contributions. France stands as perhaps the most successful example of eliminating medical bankruptcy entirely, though this comes with the trade-off of significantly higher tax burdens that some citizens find challenging.
Japan
Countries where patients still need to pay a certain amount of fees or where there is a cap to a patient’s medical expenses include Japan, where patients pay 30% of the fee. All developed nations but the US have universal healthcare, which includes South Korea, Japan, Australia, and so on. While Japan maintains universal healthcare coverage, the requirement for patients to pay thirty percent of medical costs can still create financial pressure for families facing serious illnesses or chronic conditions. This cost-sharing model, while more manageable than the American system, still forces Japanese families to consider the financial implications when making healthcare decisions, particularly for expensive treatments or long-term care needs.
